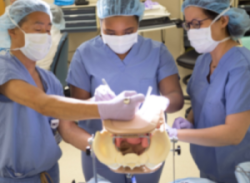
Surgical residency has been defined by the need to develop hands-on proficiency in a field where every mistake carries real consequences. As surgical techniques and patient safety standards have grown, a need for increased training in a safe environment has developed. Today, simulation training is filling the space between what residents learn in the classroom and what they need to perform with accuracy in the operating room.
At Miyazaki Enterprises, we developed the Miya Model specifically to address this challenge in women’s health surgery. Replicating the anatomical realism of live procedures, the Miya Model gives OB/GYN residents, urogynecology fellows, and surgical educators a platform to build muscle memory, refine technique, and reduce the learning curve prior to operating on a patient.
Exceptional Education Between Classroom Theory and the OR
Medical education does a superior job of teaching anatomy, pathophysiology, and clinical decision-making. It was missing the hands-on tactile, spatial, and kinesthetic experience of surgery itself. Reading about a retropubic sling placement is categorically different from navigating the Urogenital diaphragm with an introducer needle in hand.
The inherent disconnect has measurable consequences. Studies consistently show that residents who receive guided simulation training demonstrate faster skills, fewer intraoperative errors, and higher confidence scores than those trained through observation alone. Simulation accelerates the surgical experience.
Three Ways the Miya Model is Designed to Increase Resident Competency
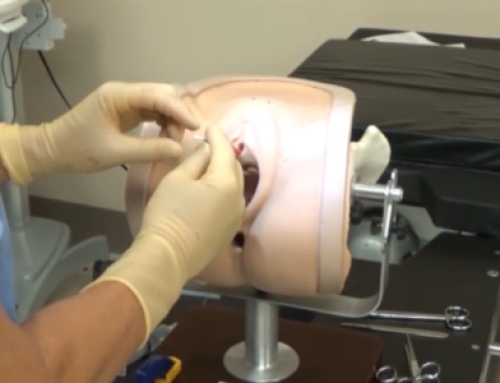
The Miya Model was designed with one goal in mind: to make simulation training as close to a live surgical case as possible. Here are three core ways it accomplishes that:
- Anatomically Accurate Tissue Resistance. The physical resistance of actual human tissue is one of the most difficult aspects of procedural training to replicate. The Miya Model closely mirrors the force metrics encountered when piercing through the Urogenital diaphragm and Obturator membrane, which are the same structures surgeons navigate during Transobturator and Retropubic sling placements. Residents develop the tactile intuition that comes only from repeated, realistic repetition.
- Full-Thickness Vaginal Dissection. Many simulation models compromise on anatomical depth, offering surface-level approximations that don’t prepare residents for the complexity of actual dissection. The Miya Model features full-thickness vaginal dissection in a structure that mirrors live surgical anatomy. Residents can practice all major sling approaches, including Retropubic (both bottom-up and top-down) and Transobturator (inside-out and outside-in) within a single model, developing procedural fluency across technique variations.
- Guided Video Instruction Through the Miya Model App. This helpful app provides residents with guided video tutorials for sling surgeries, allowing them to review technique, reinforce procedural steps, and self-assess at their own pace. The on-demand access to expert guidance extends training beyond the simulation suite and into the broader rhythm of residency, accelerating competency.
Why It Is Important For Women’s Health Surgery
Stress urinary incontinence affects an estimated one in three women at some point in their lifetime, yet it remains significantly undertreated, in part because of barriers to surgical access and in part because of the technical demands placed on surgeons who perform these procedures. Midurethral sling surgery is among the most effective and durable treatments available, but it requires precise anatomical understanding and procedural confidence to deliver consistently strong outcomes.
When residents arrive in the OR having already practiced these approaches in a simulation environment, the clinical benefit extends beyond the individual surgeon. Procedural confidence translates directly to calmer, more deliberate decision-making under pressure, a quality that is difficult to teach in a lecture hall but develops naturally through repetition in realistic training conditions. Procedures become more efficient, complication rates decrease, and patient outcomes improve across the board. With less time spent on corrective guidance and more time advancing the resident’s overall surgical development, a more productive and focused learning environment is created for everyone in the room. The surgical pipeline for women’s pelvic health is strengthened by a generation of providers who trained smarter, not just longer, and whose patients are better for it.
Simulation Is Becoming a Forward-Moving Standard
Programs that integrate simulation training into residency curricula are raising the bar. They are investing in a model of education that respects both the complexity of surgery and the well-being of the patients who depend on it. This ensures that the first time a resident performs a procedure on a patient, it is not also the first time they have understood the feel of the resistance of tissue, the angle of approach, and the intuitive muscle memory that only comes from doing. Residents who train on high-fidelity models like the Miya Model enter the OR with a level of preparedness that was simply not possible a generation ago, and programs that embrace this shift are producing surgeons who are better equipped from day one. The Miya Model was built on this principle and it is the foundation that makes surgical experience more meaningful, with accelerated competency that benefits residents, programs, and most importantly, patients.
Learn more about the Miya Model and explore simulation training resources for your program at miyazakienterprises.com.